On 4 November 1986 a momentous operation took place for the first time in the UK. A person awaiting a heart transplant was running out of time, so the medical team, led by Sir Terence English, decided to implant an artificial heart, the Jarvik-7.
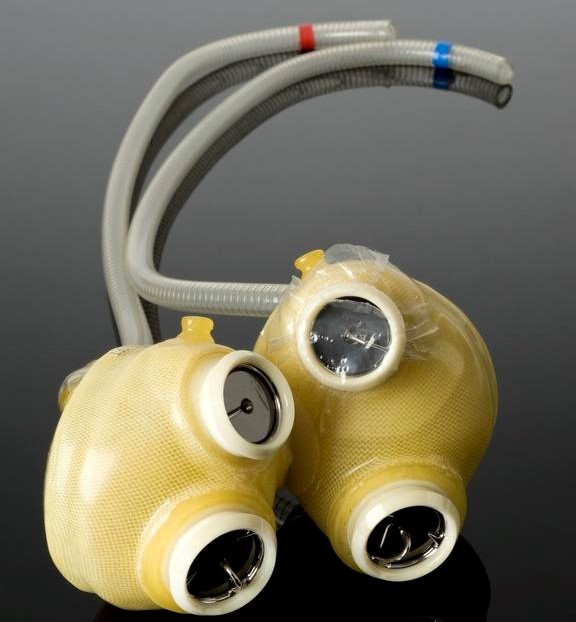
In the early 1980s an American physician named Robert Jarvik (b.1946) developed a plastic and Velcro pump that replicated the lower two chambers of the heart. It was ‘pumped’ by compressed air, and monitored by cumbersome 1980s computers.
Jarvik worked with, and was inspired by the work of, Willem Kolff (1911-2009). Kolff worked on a number of artificial organs, including a kidney dialysis machine which he developed during the Second World War, while in German-occupied Holland. He used easily available resources such as cellophane sausage casing and empty food tins to build his ‘kidney’, which served to filter the blood. This example in our collection is made from an apricot tin.

In 1982, following the first successful implantation of the Jarvik heart into 61 year old dentist Barney Clarke, Jarvik requested to meet with Sir Terence English to see if the artificial organ could be used in Papworth Hospital’s NHS transplant programme. English consented, but only as a bridge to transplant, and he and his colleagues were trained for many months by Kolff and several members of Jarvik’s team. Funding for the training and the device including the computer console came from an American medical organisation, Humana .
Once everything was in place, the team at Papworth had a long wait for a suitable patient. The Jarvik 7 is a massive device, so they needed a patient with a large chest, and in 1986 a suitable person was admitted. Although in very ill health, while waiting for a donor heart, the patient and his wife both consented to the operation.
As with any new innovation in surgery, it was difficult to fully prepare those undergoing the operation for the potential risks involved. I’ve often thought about people who consent to procedures and operations which are happening for the first time, and the massive amount of trust they place in their surgeons, especially in the face of life-threatening conditions.
In his autobiography Follow Your Star: From Mining to Heart Transplants – A Surgeon’s Story English wrote:
“The operation went smoothly…and it was a fascinating experience to have such total mechanical control over the blood being pumped around the body.”
This type of operation is known as a ‘bridge to transplant’ operation, bridging the time until a heart becomes available for transplant. It’s not an implantable heart, but a circulatory support. The patient of that historic UK first operation improved, and had a human heart transplanted two days later. English admitted:
“It was a difficult decision, as I would have liked the patient to have benefited more before transplanting him. But I knew how difficult and unpredictable it was to obtain suitable donors and so I went ahead and we took the Jarvik heart out and put the human donor heart in. The patient did well but sadly died nearly 2 years later from an infection.”
English never used the Jarvik system again, as it was much too cumbersome, expensive and meant two massive operations for the patients.

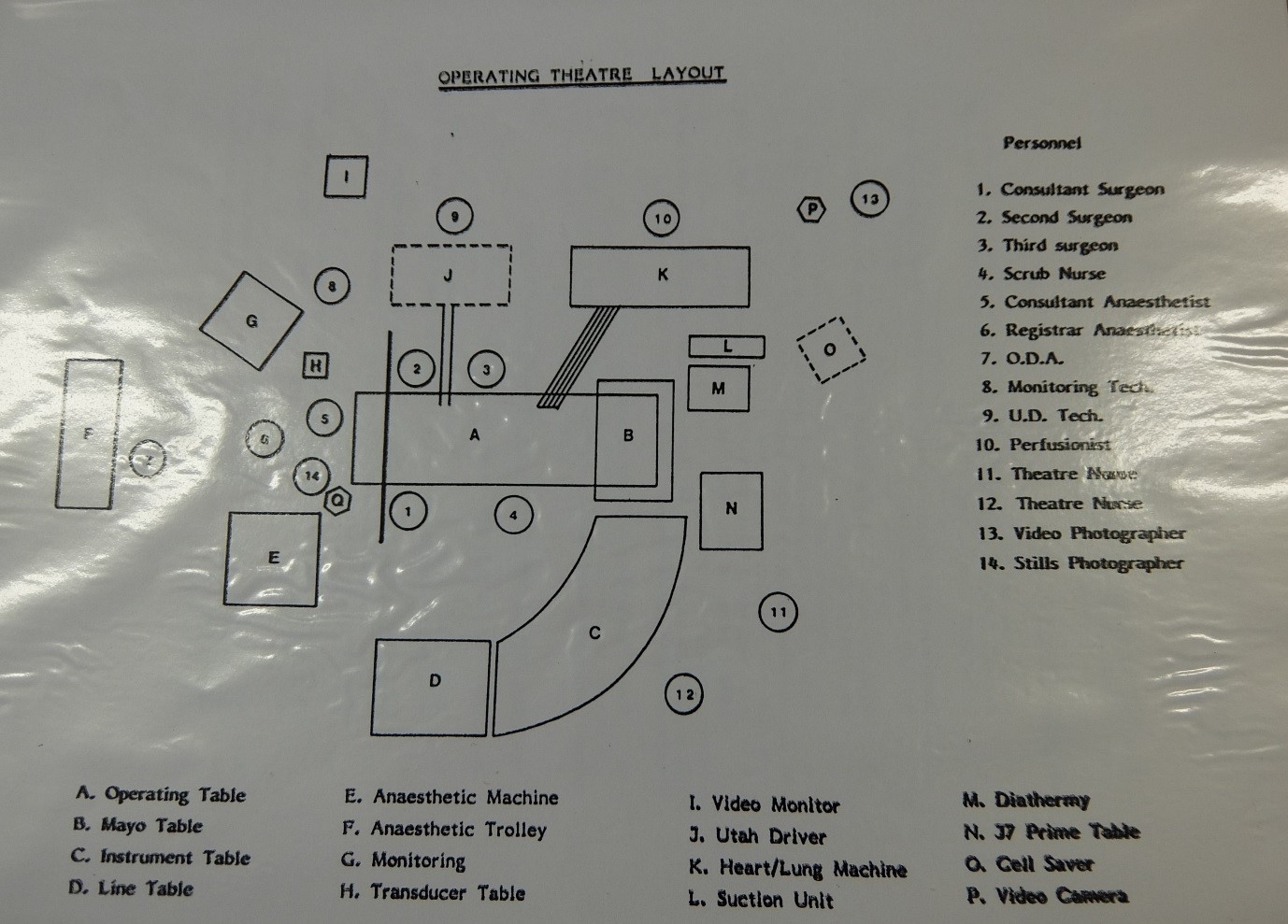
Alongside the kit, we also are incredibly fortunate to have in our collection Terence English’s ‘Artificial Heart Protocols’ documents, used during his training sessions and subsequent operation at Papworth hospital.
The manual includes details about the operation, the roles of the surgical staff including the scrub nurses, post-operative care and also the set-up of the operating theatre.
In 1981, a Scientific American article by Robert Jarvik predicted that it would be a decade until artificial hearts are routinely implanted into humans. He acknowledged the limitations of the Jarvik 7; being tethered to large machines, being uncomfortable and a risk of infection where the pumps were attached into the chest.
Thirty years on from Jarvik’s prediction, the first person in the UK to receive a completely implanted artificial heart was also treated at Papworth. Matthew Green, carried a small shoulder bag which powered his life saving pump, known as a Total Artificial Heart, meaning he could leave his house for up to three hours at a time. Mr Green used this device for two years until he received a donor heart.
With thanks to Sir Terence English for his insight into this historic operation and the kind donation of the Jarvik 7 device.
Jarvik’s prototypes are currently on display at the National Museum of American History in Washington, D.C.